Monday, February 24th. I have been in the hospital for 4 days now. I woke up to the increasing sound of doctors, residents, pain teams, and all other medical personnel who start their day around 7:30. The nurses were changing shifts, and I was wondering who I was going to get. Usually the new day nurse will come in right around then to just pop in and say hello. Mine did not, but the first people to arrive in my room were the residents of Dr. Olson's orthopedic team. There were 4 of them and they looked me over, changed my dressing for the first time (I did NOT look), and pulled my drain. I was in a lot of pain since they were poking and prodding around the incision, but was able to catch my breath quickly and relax those muscles. I am so thankful to have my mom here because each night either her or Ben have been able to spend the night at the hospital, and I really need that right now. As 2 of the residents were working on the incision, one was talking about what they were doing, and what their plans were for our next steps. Well, there was no way I could focus on what he was saying, as I was trying to breath deep and focus on controlling my muscles while the others worked around the incision. Mom was able to take in what he was saying and fill me in once they were gone and I was relaxed.
My epidural had been turned off at 6 and now it was pain control's turn to come in and pull the needle out of my back. Christina (who has seen my epidural a few times now due to issues with it directly after surgery) came in and asked if I could roll over. You would not believe how difficult it is to roll over when half you pelvis is broken. She makes it sound so easy. I looked at her and said, no. I looked above me at the traction bar I have (looks like a hanging triangle) and said I was going to lift up and that she could get it that way. No ifs ands or buts. She was doing it my way. She raised the bed so it would be easier to reach the bar and I did a full chin up. Good thing I've been working out right up until surgery, because those arm muscles definitely helped! Once the epidural was out, I was able to lower myself down again and let the muscles relax. 2 jobs complete and it's not even 9:00!
Finally at 8:30 my nurse comes in. Disappointing. It is the same nurse I had yesterday and did not like. I didn't mention her in my last post because I was hoping to be done with her, but nope, here she was again. So quick reason why I didn't care for her on Sunday- she was inattentive. She also informed me that she was "confused by my chart" and then would avoid coming in my room unless she was called in. I went 3-4 hours between her visits! So here we are, day 2 with my least favorite nurse. Once again, she avoided my room all day. She was confused by my surgeon's orders because she had never seen the mixture of medications he was requesting for me and instead of calling his team or asking for him, she ignored them ( Dr. Olson had told me exactly what medications and when I was going to take them) and did her own thing. Boy was I pissed! So here I was, off the epidural which was still slowly going out of my system and she was not overlapping medications like he had asked. Dr. Olson's main concern for his patients seems to be pain control. He says there is no reason to be in pain if we can help that with medication. So on Sunday he had requested my nurses start weaning me off of the epidural by slowly turning it down every few hours. And while they were doing that, he wanted the short acting oxy to be started in a small dose. So by the time my epidural was out of my system the Oxycontin was already in there, and I wouldn't have a hard time in between from being taken off one and started on the other. But no. My nurse did not do that, and only started the Oxycontin after the epidural was completely removed.
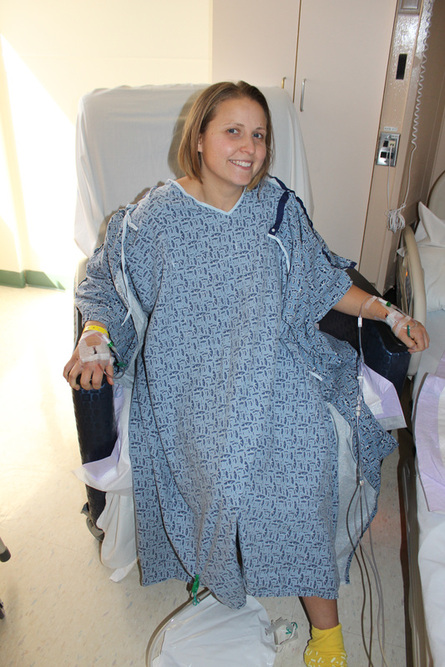
Pain was manageable, but did go up and down throughout the day. At 11 I saw occupational therapy, and stood for the first time. It felt good (and very scary)! She showed me how to shimmy on my right leg (the good one) while holding on to a walker and move to a chair. It should be easy to do this downstairs in our home because we have hardwood floors. Carpet would be much harder! So I got in a chair for the first time and was able to sit for a few hours! I even was able to get my back washed where the epidural tape was all up and down from my shoulders to my tailbone.
At this point, I hadn't seen my nurse since 10:30 when she gave me both long acting and short acting Oxycontin as well as Tylenol. I was still hooked up to a Picu (a line with a pump that I can push for an extra dose of medication) but she had told me not to press it today because she was weaning me off of it, and had even hung it up out of reach instead of the usual placement on my lap.
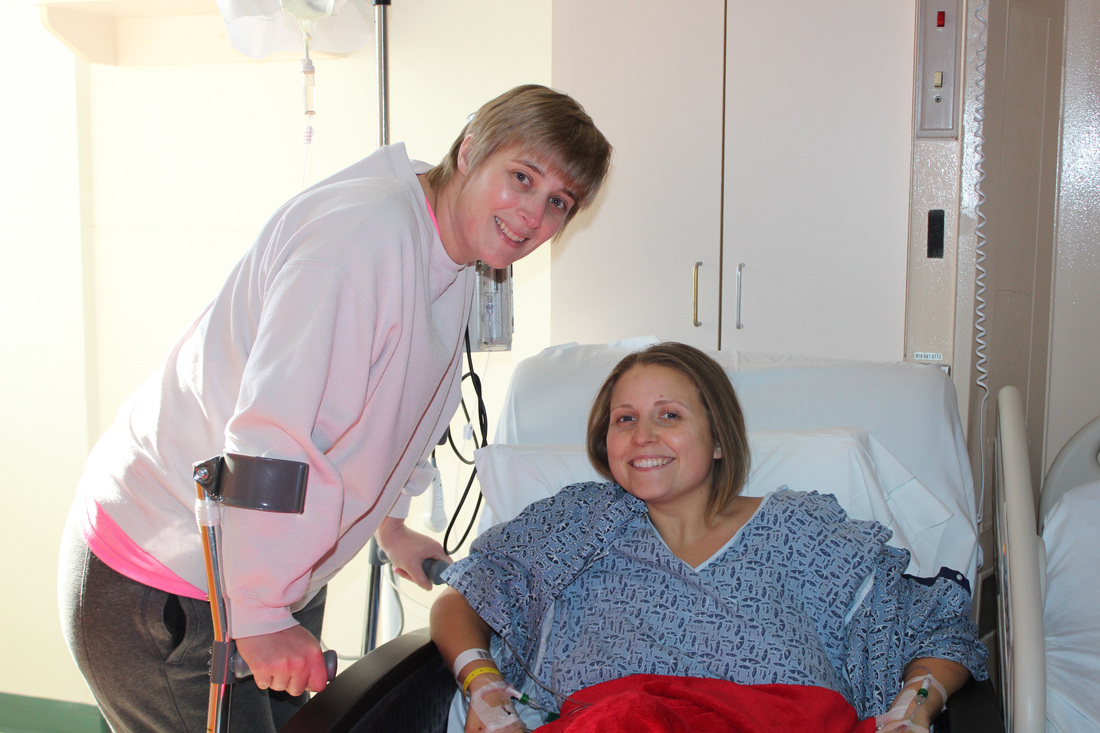
So in comes the best part of my day- Kristy is a friend I made about 2 months ago, when we were both commenting on the same Facebook post in the FB group for Periacitabular Osteotomy. We quickly realized that we were both seeing the same surgeon and that our surgeries were fairly close together. Hers was 2 and 2 days before mine. I'm sure this doesn't happen very often, especially for a surgery that is very unknown to the average person, but I was able to meet Kristy on day 4 of her post op and she and her husband stopped my today on my day 4 as she had a follow up appointment with one of Dr. Olson's team members. It was absolutely wonderful seeing her again today and seeing how much progress she has made in just over 2 weeks. It gave me encouragement and hope after seeing how far she has come.



 RSS Feed
RSS Feed
